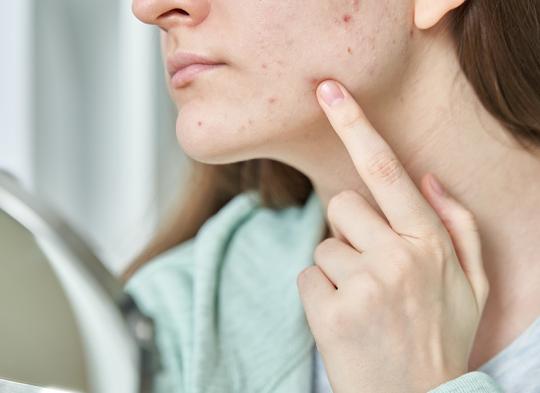
Adult acne, medically known as acne tarda, follows very different rules from the acne many people experienced during their teenage years. While adolescent skin is usually more resilient and primarily struggles with excess sebum production in the T-zone (forehead, nose, chin), mature skin reacts differently.
In adults, inflammatory lesions most commonly appear in the “U-zone,” which includes jawline, chin, and neck. The challenge is that adult skin is thinner, regenerates slower, and requires more carefully selected treatments. Using inappropriate products often leads to irritation and damage to the protective barrier, which paradxically worsens the condition. Proper skincare for adult acne should focus on rebuilding skin barrier and calming inflammation.
Specialist dermatological diagnostics allow for precise identification of the underlying causes of adult acne and implementation of targeted pharmacological therapy. In our dental and medical clinic in London, doctors develop treatment plans designed to reduce inflammation and regulate sebaceous gland activity, helping to prevent permanent scarring and hyperpigmentation. A medical consultation also provides access to treatment methods not available in standard cosmetic care.
Which nutrients are essential for good skin care?
Healthy look of adult acne-prone skin largely depends on what we have in our daily diet.
One key element is zinc, which directly reduces inflammation and helps control excessive sebum production. B vitamins are equally important, as they stabilize epidermal barrier and regulate keratinization process, preventing clogged pores. Without adequate levels of these nutrients, skin becomes more prone to irritation and responds poorly to cosmetic treatments.
Omega-3 fatty acids are another essential component. They maintain elasticity of cell membranes and help preserve internal skin hydration. Iron also deserves attention, although its role is often overlooked. Iron is responsible for oxygen transport to cells, which is crucial for efficient tissue regeneration. When iron levels are low, post-acne lesions heal more slowly, and the risk of persistent discoloration increases.
The most common mistakes in mature skin care
Aggressive cleansing and excessive exfoliation
Many people mistakenly believe that the more intensely they cleanse their skin, the better it will absorb anti-aging creams. Using heavily foaming cleansers or mechanical scrubs with large particles damages hydrolipid barrier, which is already weakened in mature skin. This leads to chronic dryness, making fine lines more visible and causing redness or irritation when introducing new products.
Skipping year-round sun protection
UV radiation is responsible for approximately 80% of visible signs of skin aging. Skipping SPF on cloudy days or during autumn and winter is one of the most common mistakes that undermines even the most expensive rejuvenating treatments. Sun exposure breaks down collagen fibres and causes hyperpigmentation, which is far more difficult and costly to treat than preventing it with daily protection.
Using too many active ingredients at once
Introducing retinol, vitamin C, and high concentrations of acids simultaneously is a fast track to severe irritation and inflammation. Mature skin needs time to adapt to stronger substances. Constantly experimenting with new products creates chaos in the routine, preventing proper regeneration. Instead of working synergistically, active ingredients may start to counteract or irritate the skin.
Neglecting the neck and décolletage
Skin in these areas is significantly thinner than on the face and contains fewer sebaceous glands, which means it ages faster. A common mistake is limiting skincare to the jawline. Without proper hydration and sun protection, the neck quickly becomes loose and wrinkled, creating a noticeable contrast with well-maintained facial skin.
How to apply skincare products
Effectiveness of skincare products depends directly on the order in which they are applied. Using the wrong sequence can prevent expensive active ingredients from reaching the epidermis, as they may be blocke by the barrier created by another product. The basic rule is based on texture: always start with the lightest, water-based formulas and gradually move toward heavier, oil-rich products.
Step one: cleansing and toning
Very important is thorough cleansing to remove impurities and allow active ingredients to penetrate effectively. Toner or essence should be applied to dry or slightly damp skin. These products restore the proper pH and enhance absorption in subsequent steps. Applying serum to overly dry, tight-feeling skin reduces its effectiveness.
Step two: serums and active ingredients
This is the stage for lightweight, water- or gel-based products such as vitamin C serum, hyaluronic acid, or peptides. If using more than one serum, start with the thinnest formula. Active ingredients in these products have small molecules that need direct contact with the skin to work effectively. Applying them over a rich cream would be ineffective, as oils create a barrier that blocks penetration.
Step three: moisturizing and protection
Moisturizer plays an occlusive role, forming a protective layer on the skin’s surface to prevent water loss and “seal in” previously applied serums. In the morning routine, the final step must be SPF. Sunscreen is designed to remain on the surface as a protective shield and should not be layered over with anything except makeup. In the evening, a facial oil may be used as the final step to further reinforce the lipid barrier.
Ingredients that should not be combined
Improperly combining active ingredients can cause severe irritation or completely neutralize their effects. Some ingredients only work within specific pH ranges and mixing them may render them ineffective or overly harsh.
Retinol and AHA/BHA acids
One of the most serious mistakes is using retinol (vitamin A derivative) together with exfoliating acids such as glycolic, mandelic, or salicylic acid in the same routine. Both groups stimulate cell renewal and can be irritating. Their simultaneous use significantly increases the risk of damaging the hydrolipid barrier, leading to burning, peeling, and inflammation.
To avoid this, acids and retinol should be used on different days or separate evenings.
Vitamin C and exfoliating acids
Combining pure vitamin C (ascorbic acid) with AHA or BHA acids is also risky. Vitamin C in this form is highly unstable and requires a low pH to remain effective. Adding additional acids may destabilize the formula, making it inactive, or excessively lower the skin’s pH, resulting in redness and irritation. The safest approach is to apply vitamin C in the morning to support sun protection and use acids in the evening.
Retinol and Vitamin C
Although both are considered gold-standard anti-aging ingredients, applying them in the same routine can be too intense. Vitamin C works best in an acidic environment, whereas retinol prefers a near-neutral pH. Used together, they may neutralize each other or intensify dryness. The golden rule is to apply vitamin C in the morning and retinol only at night.
When should you see a dermatologist?
At-home care has its limits and often cannot replace a professional medical diagnosis. Certain warning signs indicate the need for pharmacological treatment or specialist evaluation.
No improvement despite consistent care
Time is a key factor. If you have followed a well-structured routine for at least three months using proven active ingredients, such as azelaic acid or niacinamide, and protecting the skin barrier yet see no improvement, it is time to seek consultation. Dermatologist can assess whether prescription treatments such as topical antibiotics or stronger vitamin A derivatives are necessary.
Painful deep lesions
If deep, painful nodules or cysts do not respond to over-the-counter products, a medical advice is essential. These inflammatory lesions develop in the deeper layers of the dermis and carry a high risk of permanent atrophic scarring. Early intervention can stop inflammation before irreversible structural damage occurs.
Scarring and persistent hyperpigmentation
If each new lesion leaves a lasting mark, whether a red post-inflammatory spot or a visible indentation, do not delay seeking help. Dermatologist can implement therapy that accelerates healing and prevents new lesions, reducing the need for costly aesthetic treatments in the future.
Suspected hormonal causes
In adults, acne is often linked to endocrine disorders. If breakouts concentrate along the jawline and neck, worsen before menstruation, or are accompanied by other symptoms such as excessive hair growth or irregular cycles, dermatologist may recommend hormonal testing or referral to an endocrinologist. Treating acne without addressing its hormonal cause rarely gives lasting results.
Summary
Effective care of adult acne-prone skin requires abandoning aggressive drying methods in favour of rebuilding protective barrier and precisely calming inflammation. Although well-chosen active ingredients and correct product layering can significantly improve skin’s appearance, home care is often insufficient in cases of hormonal imbalance or deep inflammatory lesions.
If your current routine does not deliver results or breakouts are recurrent, seeking medical advice is the most effective next step. Professional diagnostics and targeted pharmacological treatment can regulate sebaceous gland activity, reduce inflammation, and restore healthy-looking skin.